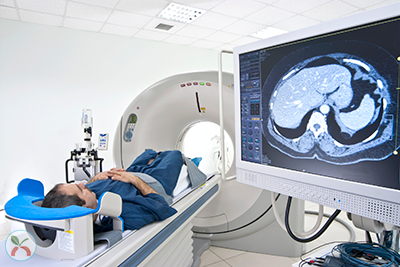
When the young Eric Dishman started experiencing fainting spells 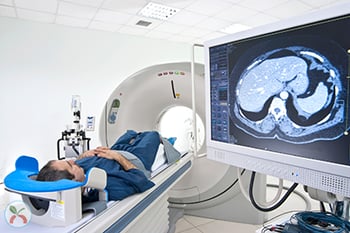 more than two decades ago, he needed answers. So he went to see a doctor.
more than two decades ago, he needed answers. So he went to see a doctor.
But those answers weren't easy to get. For six months, he endured a long list of appointments and diagnostic tests with six different doctors. None of them appeared to be on the same team, even though his digital file of electronic health records was expanding. Something was missing.
Sound familiar? More tests. More electronic health records. Another diagnosis. More medication. It's the typical approach used to treat patients. And it may be time to rethink this model of care.
Why? Playing the game of patient care without a team is a recipe for failure. Electronic health records can provide healthcare professionals with data to help people, but it’s not enough to win the game against chronic disease.
There’s another key player in healthcare that’s critical to patient care: health risk assessment data.
What if healthcare functioned more like a team sport to treat patients instead of a disconnected solo performance?
Health risk assessment data can help connect patients and providers to improve care and control costs, but there’s still work to be done to make this a universal practice.
Dishman's experience opened the door to a new way of thinking about the current healthcare delivery model. Here's what happened:
 When his doctors did finally meet for the first time, they could only agree on a few things by looking at his electronic health records.
When his doctors did finally meet for the first time, they could only agree on a few things by looking at his electronic health records.
And the news wasn't good. Cancer-like cells were attacking his immune system and slowly destroying his kidneys. He'd never be eligible for a kidney transplant, and he probably wouldn't live longer than two or three years.
Unfortunately, they hadn't spent a lot of time comparing notes. So each doctor only understood a small part of what was really happening. And no one had enough information to know how to effectively treat him—information a health risk assessment could have provided about his overall health, lifestyle, diet, activity level, risk for disease, and other factors.
But what if every doctor studied Dishman's HRA data and thoughtfully compared notes before ordering another test?
It's a question Dishman has thought about for the last 20 years. He's alive and well, received a kidney transplant, and is among a small group of thought leaders in healthcare technology with a vision to make healthcare a team sport by getting healthcare professionals to look at HRA data and Electronic Health Records. Here's how:
Use data and technology
Every day more and more people are tapping into technology to manage their health. For example:
- A doctor can manage a patient's blood pressure, glucose levels, sleep habits, and many other vital signs remotely.
- An estimated 7 million doctor-patient sessions will take place remotely via telemedicine in 2018.
- DNA testing and genome sequencing can provide highly customized data about a patient's overall health and risk factors for disease.
- There's no shortage of apps and mobile devices that can help doctors collect data about a patient without an actual in-office visit.
- And health risk assessment data can provide a patient's entire healthcare team a complete snapshot of their lifestyle habits, risk factors for disease, and medical history to help make decisions about care and treatment.
Task a group of healthcare providers, doctors, specialists, and practitioners with working together as a team to treat a patient, and data and technology will bring them together.
 Encourage patients to be proactive
Encourage patients to be proactive
When Dishman got the news about his "terminal" condition, he felt terrible. It seemed like his only option was to follow the schedule, give up, and die in a couple of years.
But something happened that changed his mind, and his perspective on the doctor-patient relationship.
"An older woman I met in the hospital grabbed me after I got the news," says Dishman. "She took me to the medical library and helped me research diseases and diagnosis. We learned that people with my condition are typically in their 70s or 80s, and doctor's probably didn't know a lot about how to treat this in a young person. And that's when she told me, 'Wake up and take control of your health, and get on with your life."
Team player or passive patient?
Based on the current healthcare system, patients aren't encouraged to be team players. Instead, it's a model designed for patients to passively wait for a diagnosis and follow a given treatment plan without asking any questions, says Dishman.
But it doesn't have to be that way. If patients learn to access available volumes of research, data, and information to learn more about their health, they can ask questions and engage their healthcare team to achieve the best outcomes.
For example, when someone completes a health risk assessment, it provides personal health information that can motivate that person to make lifestyle changes, or seek medical care.
When patients are proactive about their health, it's an easier path to prevent disease, manage existing conditions, and ultimately control healthcare costs.
Team up to improve healthcare
"The doctor-patient, one-on-one visit at a hospital or clinic is a relic of the past," says Dishman. "I want to use technology to make healthcare a coordinated team sport."
When that happens, it opens the door to promote health, prevent disease, improve quality of life and patient care, and control skyrocketing healthcare costs.